Goals & Challenges
Goals for Digitally Enabling Universal Health Platform to Meet SDG 3 Targets
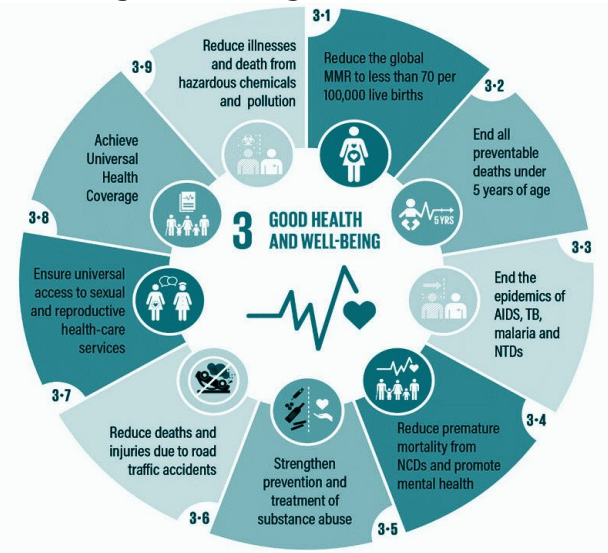
Commitment to SDG 3 Goals
By achieving these goals, the platform aims to deliver universal healthcare, advancing towards meeting or exceeding the United Nations Sustainable Development Goal 3 for good health and well-being for all. This initiative will strengthen healthcare systems, improve health outcomes, and enhance the quality of life across the nation.Digital Health Infrastructure Goals
- Citizen Health Portal: Develop a detailed, secure, and up-to-date portal for citizens to access their health records, improving the management and tracking of personal health.
- Standard Clinical Protocols: Establish standard protocols for primary, secondary, and tertiary care to ensure consistent and quality healthcare services nationwide.
- Integration of Health Insurance and Preventive Programs: Connect all government health insurance and preventive health programs into a unified platform to streamline access to benefits.
- Centralized Asset and Pharmacy Management: Build a centralized system to manage healthcare assets and pharmaceuticals, optimizing resource availability and reducing shortages.
- Telemedicine and Tele-ICU: Enable telemedicine and tele-ICU services to improve access to specialized care, especially in remote or underserved areas.
- Public-Private Integrated Health Delivery Program: Expand healthcare access by integrating public and private healthcare providers, making health services more widely available and accessible..
Challenges in Delivering Universal Healthcare
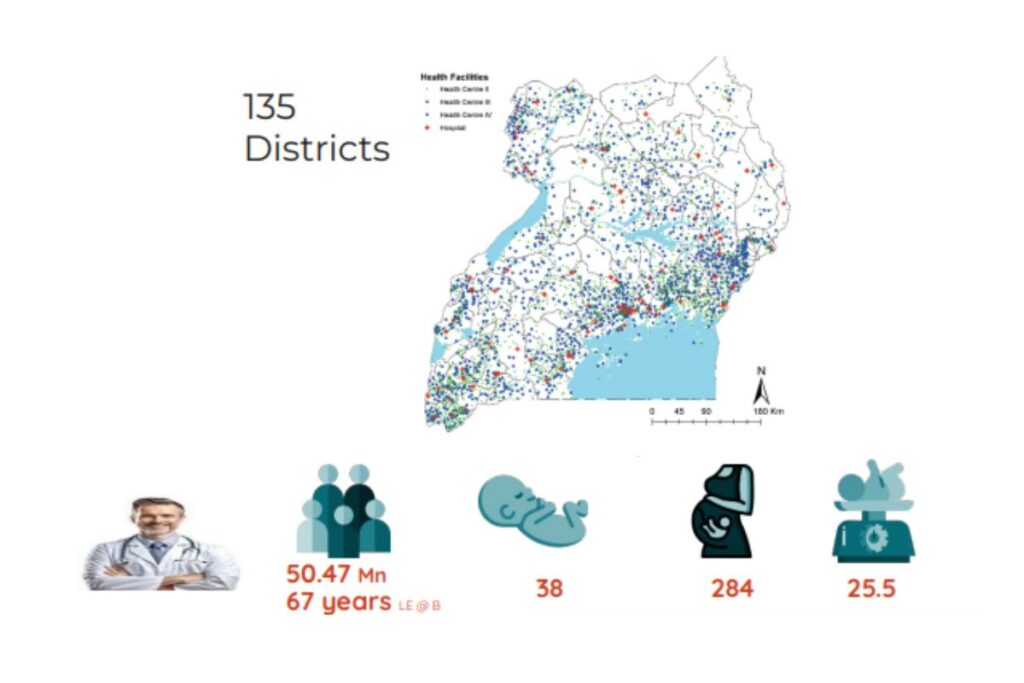
Access to care
- Provider Availability: Currently, there is only 1 doctor available for every 25,000 people, highlighting a significant shortage of medical professionals.
- Travel Distance: Patients often need to travel long distances to reach healthcare facilities, which is a considerable barrier for rural and remote communities.
- Resource Scarcity: There is a lack of essential drugs and equipment, limiting the capacity to provide effective treatments.
- High Out-of-Pocket Costs: Patients face high personal expenses for medical care, making it less accessible, especially for low-income groups.
Intersectoral Coordination
- Fragmented Programs: Many healthcare programs operate in silos, lacking integrated efforts that could optimize resource utilization and enhance service delivery.
- Isolated Systems: Standalone applications and databases hinder seamless data sharing and communication across departments.
- Lack of Alerts and Reminders: The absence of a system for automated alerts and reminders affects timely care, particularly for chronic diseases requiring regular monitoring.
Capacity and Infrastructure
- Device and Network Shortages: There is an insufficient supply of medical devices and a limited network of healthcare facilities, constraining the healthcare system’s capacity.
- Inadequate Support Systems: The support available for healthcare professionals is limited, affecting their ability to provide efficient and effective care.
- Skill Gaps: A lack of continuous skill-building opportunities for healthcare providers impedes their ability to deliver specialized and updated care.
Citizen Empowerment
- Awareness Deficit: Many citizens are unaware of available government healthcare programs, which could offer them free or subsidized care.
- Complex Medical Decision-Making: Patients often face difficulty in understanding complex medical information, impacting their ability to make informed decisions.
- Education Barriers: There is a general lack of patient education, which can lead to poor health-seeking behavior and adherence to treatment.
- Marginalized Populations: Tribal and other underserved populations experience additional challenges due to geographical and social barriers.
Monitoring and Evaluation
- Impact Studies: There is a need for continuous studies on the impact of best practices to ensure that healthcare initiatives are delivering desired results.
- Standardization and Automation: Standardized protocols and automated systems for care management could improve consistency and efficiency in healthcare delivery. Motivation and Rewards: Efforts to motivate healthcare providers and reward improvement are essential for sustaining quality care and encouraging best practices.
Healthcare Infrastructure Overview
Population Served: 50.47 million people with an average life expectancy of 67 years.
Healthcare Facilities:
- 4 National Referral Hospitals
- 5 Specialized Hospitals
- 112 General Hospitals
- 2,217 Health Centers II
- 1,242 Health Centers III
- 191 Health Centers IV
Healthcare Workforce:
- 21,050 Doctors
- 42,321 Nurses
These challenges highlight the multifaceted barriers to achieving universal healthcare, with significant needs for resource optimization, infrastructural investment, citizen engagement, and improved healthcare policies.


The healthcare system faces a high burden of both communicable diseases and non-communicable diseases.
Top 5 Disease Burdens
- HIV/AIDS
- Tuberculosis (TB)
- Lower Respiratory Infections
- Diarrhea
- Malaria

